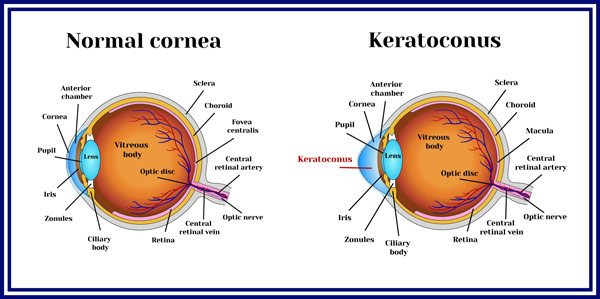
What Is Keratoconus?
Keratoconus is a condition that causes the cornea (the clear window in the front of the eye) to become thin, weak, and slowly sag over time. This change can cause progressive and substantial vision loss which requires eye surgery.
How Prevalent Is the Keratoconus Eye Condition?
Estimates of the prevalence for keratoconus range from 1 in 500 to 1 in 2,000 people. What causes keratoconus is still debated, but there is strong correlation to genetic, environmental, and hormonal factors. In rare circumstances, it can also occur after LASIK surgery (called post-LASIK ectasia).
Keratoconus Symptoms
It can take years for a cone-shaped cornea to develop in some people, where others find their condition worsens quickly. For those whose condition worsens gradually, they will typically experience mild symptoms, such as mild blurriness, vision that’s slightly distorted, swelling or redness, and increased sensitivity to glare and light.
A person with advanced disease will experience worsening vision and discomfort. Their vision will become more distorted. They will experience more blurriness, and eye conditions like astigmatism and nearsightedness will also worsen. When this occurs, a person may need to update their eyeglass prescriptions more frequently.
People who wear contacts may experience discomfort when wearing their lenses, or discover that they no longer fit. This is typically due to corneal scarring, which changes the surface on which contact lenses rest.
How Is Keratoconus Treated?
The kind of keratoconus treatment given depends both on how severe the condition is and whether it is progressing quickly or slowly. But all treatments focus on improving vision and slowing disease progression.
If a person’s keratoconus is in the mild to moderate stage of severity, a contact lens or eyeglasses are typically prescribed. For those whose keratoconus has progressed to the severe stage, corneal collagen cross-linking can be done to make the cornea stronger. This treatment can be combined with INTACS inserts, a surgical option, for even better results.
What Are INTACS for Keratoconus?
INTACS inserts are two curved, clear plastic segments that are implanted in the perimeter of the cornea to reduce nearsightedness (myopia) in patients with keratoconus. They apply pressure to the sides of the cornea, which causes it to flatten and achieve a more normal shape. INTACS inserts are available in a range of thicknesses. The thicker the insert, the more pressure it exerts. This allows INTACS implants to be used for the treatment of keratoconus at several degrees of refractive error.
Previously, these inserts were only approved for use in patients with mild nearsightedness and farsightedness. However, they have since received FDA approval to treat keratoconus.
How Is Keratoconus Surgery Performed in SLO County?
The INTACS procedure is reversible and only takes 10-20 minutes. It begins by placing numbing drops into your eyes. Then, a small incision is made into the corneal epithelium, or surface, down to what’s called the corneal stroma layer. A tunnel is created through this layer, and the INTACS inserts are inserted through the tunnel. They are then placed onto the central layer of your cornea.
When placement is complete, the surgical incision is closed by applying a small suture.
What Happens After the Procedure?
After the procedure is complete, you will be prescribed eye drops to decrease discomfort and prevent infection. The suture will be removed approximately two weeks after the procedure.
You can expect corrected vision in a few months’ time.
Who Should Consider INTACS Surgery?
INTACS inserts have been designed to improve vision over the long term in those with advanced keratoconus. They can also potentially delay the need for corneal transplant surgery. If you have been diagnosed with keratoconus and are no longer able to achieve functional vision using contact lenses or glasses, INTACS may be for you. This may also be true if your only remaining option is a corneal transplant.
You must also meet the following eligibility criteria:
- 12 years of age or older
- Progressive keratoconus or other ectatic disease
- Post-LASIK (or other corneal refractive procedure) corneal ectasia
- Fluctuating refraction after RK (+0.75D variation)
- Able to commit to a minimum of six (6) office visits (1 day; 1 week; 1, 3, 6, months) over a one-year period
- Any patient with Keratoconus age 40 or under with BCVA worse than 20/15